
The Future of SNF Claims Processing: AI, Automation, and Real-Time Claim Visibility
In today’s Skilled Nursing Facility (SNF) environment, operational efficiency is no longer a “nice to have” it is a prerequisite for financial stability and sustained patient care quality. Yet despite advances in healthcare technology, many SNFs remain buried under a daily flood of documents arriving via eFax.
Physician orders, referrals, prior authorizations, EOBs, and supporting documentation for Medicare and Medicaid claims form the backbone of the revenue cycle. When these documents are handled manually, they become a silent bottleneck—slowing claims, increasing denials, and pulling skilled staff away from patient-focused work.
Intelligent eFax automation, powered by AI-driven claims processing, is rapidly redefining this reality. By converting unstructured fax data into actionable, real-time workflows, SNFs are laying the foundation for the future of claims processing—one defined by speed, accuracy, and visibility.
The Bottleneck: Why Manual Fax Processing Fails SNFs
Manual eFax workflows require staff to visually review, sort, and route every incoming document. In high-volume SNFs, this repetitive process creates compounding inefficiencies:
- Delays in claims submission
- Misfiled or overlooked documentation
- Increased denial risk
- Reduced staff productivity and morale
When critical documents are delayed or misplaced, claims stall—and so does cash flow. Over time, this erodes SNF revenue cycle automation efforts and weakens financial performance.
Why is claims automation vital for SNFs?
Because manual processes introduce risk at the very first step of the claims lifecycle. A single missing authorization or late EOB can delay reimbursement by weeks. Automation removes this fragility by ensuring documents are captured, classified, and routed correctly the moment they arrive.
How AI Is Transforming SNF Claims Processing
How will AI change SNF claims processing?
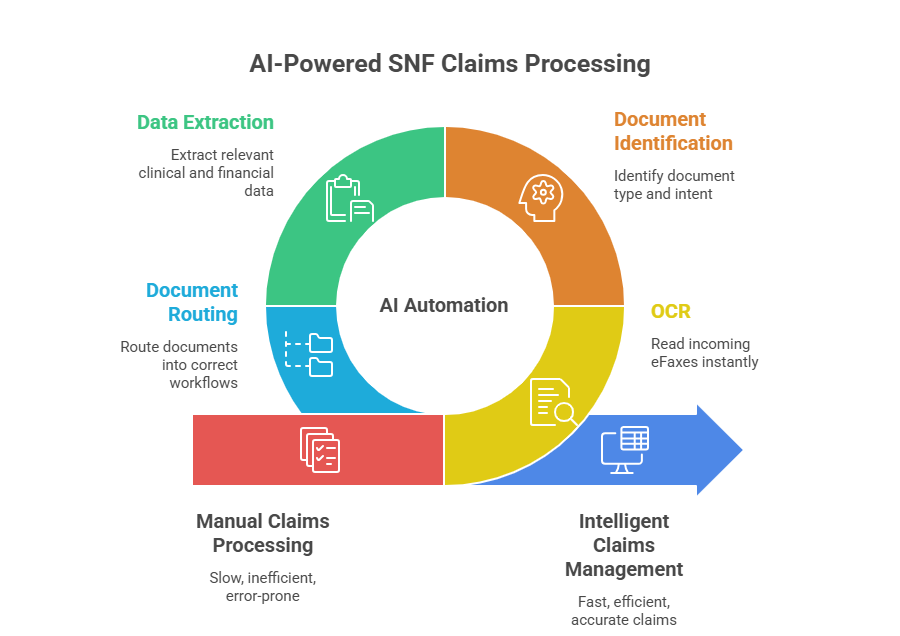
AI transforms claims processing by eliminating manual document handling altogether. Using Machine Learning, OCR (Optical Character Recognition), and Natural Language Processing (NLP), intelligent automation systems can:
- Instantly read incoming eFaxes
- Identify document type and intent
- Extract relevant clinical and financial data
- Route documents into the correct claims or EHR workflows
What was once a static fax inbox becomes a dynamic, intelligent claims management system—one that actively accelerates the revenue cycle instead of slowing it down.
The Benefits of Intelligent eFax Automation
1. Seamless Document Management and Routing
AI-powered intelligent classification instantly recognizes prior authorizations, clinical notes, referrals, and EOBs, routing each document to the correct department or system automatically. This removes delays caused by manual forwarding and dramatically reduces overall fax processing time.
2. Enhanced Compliance and Error Reduction
Automation enforces consistency. By eliminating manual sorting and data entry, SNFs significantly reduce human error—supporting compliance requirements and improving first-pass claim accuracy for both Medicare and Medicaid submissions.
3. Real-Time Claim Visibility and Predictive Intelligence
What is real-time claims visibility for SNFs?
It is the ability to track documents and claims end-to-end—from arrival to submission to payment—without blind spots.
With real-time visibility:
- Staff see claim status instantly
- Missing documentation is identified early
- Bottlenecks are addressed proactively
When combined with predictive analytics, AI can flag claims at risk of denial before submission, allowing teams to intervene early and protect revenue.
Can real-time visibility improve SNF revenue?
Absolutely. Faster issue resolution leads directly to quicker reimbursement and improved cash flow predictability.
Use Cases Shaping the Future of SNF Automation
How can SNFs use AI for claims submission?
AI can automatically assemble complete claim packets by pulling the right authorizations, clinical notes, and physician orders identified via NLP from the document stream. This reduces manual assembly time and accelerates submission readiness.
What is the future of SNF claims management?
The future is end-to-end claims workflow automation, where intake, validation, submission, and monitoring are orchestrated by AI. This replaces fragmented, manual steps with a unified system designed for scale, compliance, and speed.
Author -Pradeep Dhakne
Read our next blog – Click here

