
Redefining the Future of SNF Accounts Receivable
For Skilled Nursing Facilities (SNFs), financial sustainability is inseparable from the effectiveness of Accounts Receivable (A/R) management. In an environment defined by complex payer rules, frequent regulatory changes, and tightening margins, delayed or denied reimbursements can quickly destabilize operations. Yet, many SNFs continue to rely on legacy, manual processes to track medical claims—processes that were never designed for today’s volume, velocity, or payer complexity.
Traditional claim follow-up often involves repetitive portal checks, lengthy phone calls, fragmented documentation, and delayed responses to payer requests. These inefficiencies inflate A/R days, overburden billing teams, and create avoidable revenue leakage. In a healthcare ecosystem where speed, accuracy, and predictability directly impact cash flow, such limitations are no longer sustainable.
This is where Artificial Intelligence (AI), combined with real-time claim status tracking, is fundamentally reshaping SNF revenue cycle management (RCM). AI-enabled claim tracking delivers continuous visibility into the entire claim lifecycle, allowing facilities to identify issues early, resolve them faster, and prevent denials before they occur. What was once a reactive, labor-intensive process becomes proactive, data-driven, and strategically controlled.
AI-powered A/R optimization for SNFs is no longer an emerging concept—it is rapidly becoming a core capability for organizations seeking to get paid faster, reduce administrative burden, and stabilize revenue streams. This guide explores why traditional claim tracking fails, how AI transforms the process, and how SNFs can apply real-time intelligence to strengthen financial performance.
Why Traditional Claim Tracking Falls Short
At the heart of most SNF A/R challenges lies a fundamental lack of timely, reliable information. Manual claim tracking methods provide limited visibility and often surface problems only after financial damage has already occurred.
Delayed Issue Detection
When claims are monitored manually, stalled or rejected submissions frequently go unnoticed for days or even weeks. By the time billing teams identify an issue such as missing documentation, authorization errors, or coverage mismatches the payer’s timely filing window may already be closing. These delays prolong reimbursement cycles and directly increase A/R days.
Excessive Administrative Burden
Billing staff spend a disproportionate amount of time navigating payer portals, making follow-up calls, and documenting claim updates across disparate systems. These repetitive tasks divert skilled resources away from higher-value activities such as denial analysis, appeals strategy, and patient financial coordination. Over time, this inefficiency undermines overall nursing home billing productivity.
Revenue Leakage and Missed Opportunities
Slow resolution cycles, overlooked payer requests, and missed follow-up deadlines contribute to preventable denials and write-offs. Even small delays, when multiplied across hundreds or thousands of claims, can significantly erode SNF cash flow and financial predictability.
Lack of Forward-Looking Insight
Traditional claim tracking only reflects historical status updates. It provides no predictive intelligence to flag claims at risk of denial, identify payer-specific bottlenecks, or prioritize work based on financial impact. As a result, billing operations remain locked in a reactive mode constantly responding to problems rather than preventing them.
How AI Transforms Real-Time Claim Status Tracking
AI-enabled real-time claim status tracking represents a structural shift in how SNFs manage their revenue cycle. Instead of relying on intermittent checks and manual follow-up, AI continuously monitors claims across payers, systems, and workflows, delivering actionable intelligence in real time.
Accelerated Speed and Operational Efficiency
AI automates claim status retrieval directly from payer systems, updating claim progress continuously without human intervention. This eliminates repetitive manual tasks, accelerates claim processing timelines, and significantly reduces A/R days. Billing teams gain instant awareness of where every claim stands without logging into multiple portals.
Improved Cash Flow Predictability
When issues are identified and resolved early, claims move through the reimbursement cycle faster. Faster resolution translates directly into quicker payments and more predictable cash flow. Over time, this consistency strengthens financial planning and operational stability for SNFs.
Proactive Denials Prevention
Real-time AI alerts flag potential issues such as missing authorizations, coverage inconsistencies, or documentation gaps—before a claim is formally denied. This allows staff to correct errors immediately, dramatically reducing denial rates and preventing avoidable rework.
Centralized Visibility and Executive Control
AI platforms consolidate claim data into a single, unified dashboard, providing complete visibility across payers, claim types, and aging categories. Revenue cycle leaders gain real-time insight into performance trends, bottlenecks, and risk areas, enabling informed decision-making and targeted process improvements.
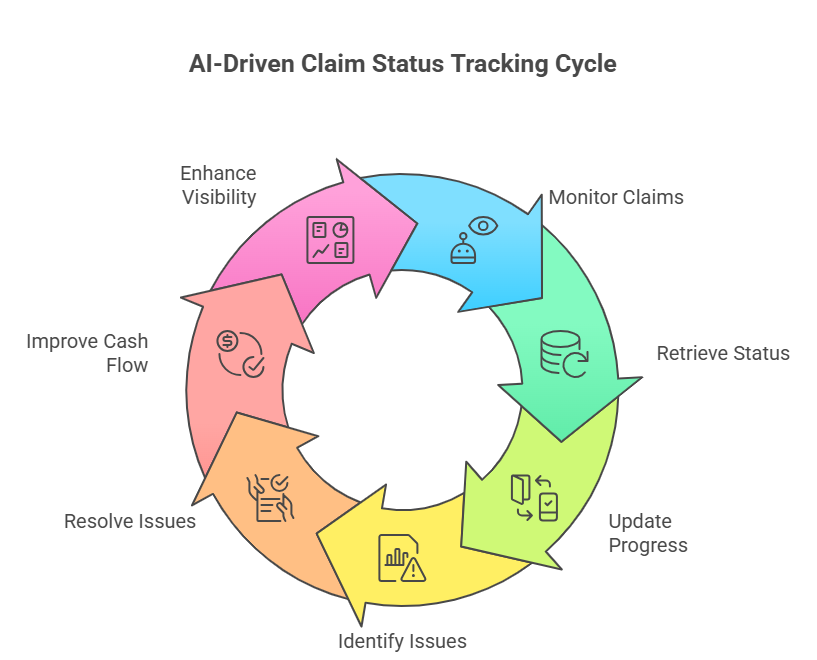
Practical Use Cases: AI-Driven Claim Tracking in Real SNF Operations
Proactive Denial Intervention
Immediately after claim submission, the AI system monitors payer responses continuously. If a claim status changes to “pending additional information,” automated alerts notify the appropriate team member. Required documentation can be uploaded within hours often preventing a denial altogether.
Payer Performance Analysis
AI-driven analytics identify recurring delays or denial patterns associated with specific payers. Armed with objective data, SNFs can renegotiate payer workflows, adjust submission strategies, or escalate systemic issues with clear evidence.
Intelligent Work Prioritization
Using predictive analytics, AI ranks claims based on risk level, expected reimbursement value, and likelihood of denial. Billing teams can focus first on high-impact claims, ensuring effort is aligned with financial outcomes rather than chronological aging alone.
Manual vs. AI-Enabled Claim Status Tracking: A Clear Contrast
| Dimension | Manual Claim Tracking | AI-Enabled Real-Time Tracking |
|---|---|---|
| Status Updates | Periodic or denial-driven | Continuous, real-time monitoring |
| Staff Effort | High manual workload | Automated, low-touch operations |
| Issue Handling | Reactive after denial | Proactive before denial |
| Data Accuracy | Variable, human-dependent | High, system-driven |
| A/R Impact | Prolonged A/R cycles | Faster resolution, lower A/R days |
From Chasing Claims to Controlling Cash Flow
In today’s high-pressure skilled nursing environment, financial resilience depends on visibility, speed, and control. Manual A/R processes, once tolerable, now represent a structural liability. AI-driven real-time claim status tracking addresses these limitations at their root eliminating blind spots, reducing delays, and transforming revenue cycle operations from reactive to predictive.
By embracing AI-enabled A/R automation, SNFs can stabilize cash flow, reduce administrative burden, and ensure that reimbursement processes support not hinder their mission of delivering high-quality patient care.
Ready to stop chasing claims and start accelerating revenue?
Discover how our AI-powered real-time claim tracking solution delivers the visibility, control, and speed your SNF needs to optimize revenue cycle performance.
Author – Nidhi Vyawahare
Read our next blog – Click here

