Prior authorization remains one of the most time-consuming administrative processes for provider organizations.
This gated resource outlines proven best practices for streamlining prior authorization, helping provider organizations reduce delays, improve accuracy, and scale operations more effectively.
Download Free Guide
Why Prior Authorization Needs to Be Streamlined
Common Challenges in Provider Authorization Workflows
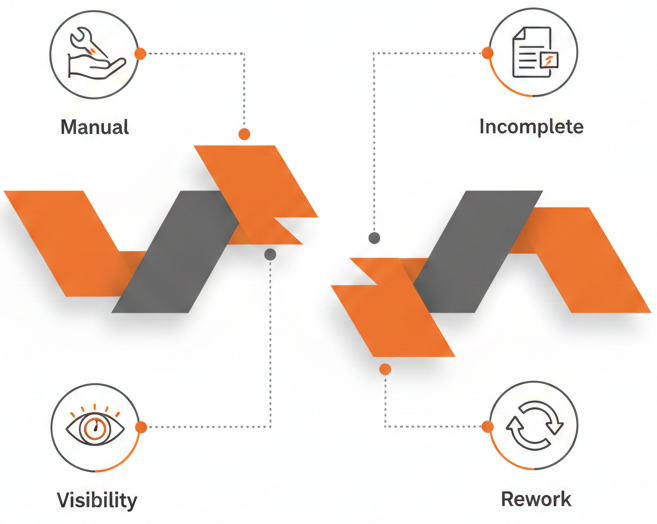
Many provider organizations face similar issues:
These challenges slow approvals and strain administrative teams.
Best Practices
Standardize Authorization Workflows
Standardizing workflows ensures that every authorization request follows a consistent process. This reduces variation across teams, improves accountability, and shortens approval cycles.
Centralize Clinical Documentation
Centralized documentation ensures that all required clinical information is accessible and complete before submission. This reduces errors and minimizes requests for additional information.
Identify Authorization Requirements Early
Early identification of authorization needs helps prevent last-minute delays. Capturing required information upfront improves submission readiness and reduces rework.
Leverage Automation and AI
Automation and AI help reduce manual effort by streamlining submissions, validating documentation, and tracking authorization status in real time. Intelligent workflows improve both speed and accuracy.
Enable Real-Time Visibility and Tracking
Real-time dashboards and alerts provide visibility into authorization status, helping teams act quickly and avoid delays caused by missed follow-ups.
Align Clinical and Administrative Teams
Clear communication and role alignment between clinical and administrative teams reduce handoff delays and improve overall workflow efficiency.
Operational Impact of Streamlined Authorization
By following best practices, provider organizations can achieve:

