Discover AI-Powered Healthcare Agents — On Your Terms
The ValueDX AI Experience Center gives your clinical and billing teams a direct, hands-on look at how prior authorization automation works in practice — not a slide deck or a scripted walkthrough. Watch Authorization CareDX, our dedicated AI agent, pull clinical documentation from your EHR, map it to payer-specific requirements, submit the request through the correct portal, and surface real-time approval status — all without a staff member touching a keyboard. If your team is currently evaluating prior authorization automation vendors, this is where workflows get tested against actual payer rules and real submission outcomes.
Why Manual Prior Authorization Keeps Failing Healthcare Teams
Manual prior authorization workflows break down at every handoff. Physicians compile clinical documentation, billers translate it into payer-specific formats, staff submit through multiple portals, and then everyone waits — with no visibility into status, no alert when a request is expiring, and no early warning when a denial is imminent. According to the American Medical Association, 94% of physicians report that prior authorization delays patient care, and 80% report that PA burdens have caused patients to abandon recommended treatment entirely. These are not workflow inconveniences — they are revenue leaks and patient safety risks that compound with every manual step in the process.
How ValueDX AI Prior Authorization Automation Works — End to End
Measurable Benefits of AI Prior Authorization Automation for Healthcare Platforms
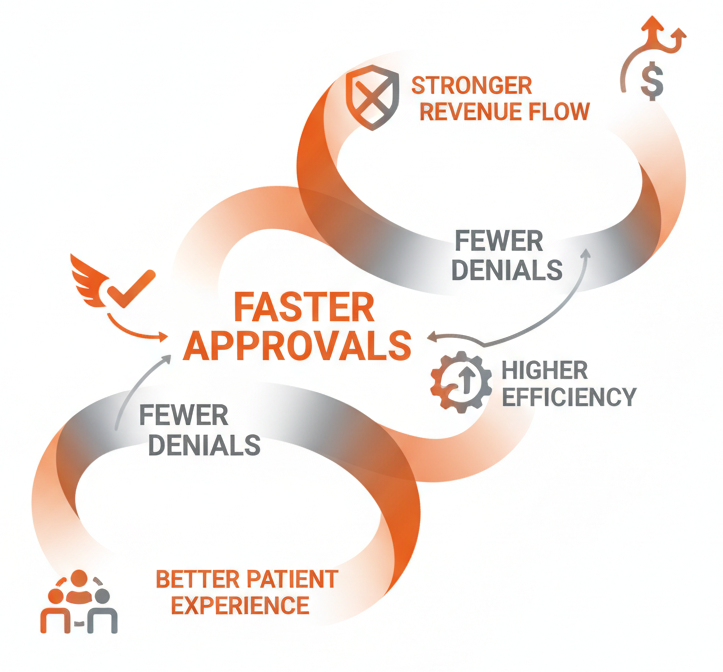
Why Healthcare Platforms Choose ValueDX for Prior Authorization Automation
ValueDX is built specifically for complex US payer environments, not generic automation. Its AI uses payer rules, clinical data, and denial patterns to reduce denials before submission. It scales across payers, specialties, and locations without adding staff.
Proven Prior Authorization Accuracy and Turnaround Improvement
Multi-Specialty and Enterprise Scalability
Analytics-Driven Prior Authorization Performance Insights
HIPAA, SOC 2 Type II, and Healthcare Interoperability Compliance
Experience the Power of Healthcare AI Agents Firsthand
See exactly how ValueDX AI-powered agents can transform your authorization management, reduce manual burden, and improve outcomes. Book a personalized demo built around your platform’s PA processes, complexity, and volume.
Fill out the form below and we’ll be in touch to schedule a convenient time.
Let’s explore how intelligent automation can transform your healthcare delivery.
Frequently Asked Questions — AI Prior Authorization Automation
Start Automating Prior Authorization Today — Book Your Personalized Demo
The ValueDX AI Prior Authorization Automation platform changes that equation — and we will show you exactly how it applies to your payer mix, your specialty, and your current PA volume. No generic demo. No slide deck. A live walkthrough of real authorization workflows, real payer connections, and real denial-prevention logic — built around your facility’s specific challenges and service lines. No obligation required.
Before You Leave…
Explore how automated prior authorization can streamline approvals, reduce denials, and speed up revenue cycle throughput.
Request a Free Consultation
