Slow Credentialing Delays Revenue
Manual credentialing processes create bottlenecks that delay provider onboarding and payments. Missing documents, human errors and repeated data entry cost time and compliance risk. ValueDX automates these workflows, ensuring each provider is enrolled accurately and on time.
Discover AI-Powered Healthcare Agents — On Your Terms
Step into the ValueDX AI Experience Center and explore how our intelligent automation solutions are transforming credentialing and provider enrollment workflows. See AI agents in action as they streamline documentation, accelerate payer enrollment, reduce delays, and ensure providers are authorized to deliver care faster
Smarter Credentialing with AI, OCR and ICR
ValueDX automates every stage of credentialing from data capture to payer approval. ValueDX AI engine extracts information from CAQH, NPPES and licensing documents using OCR and ICR, validates accuracy and submits applications automatically to payers.
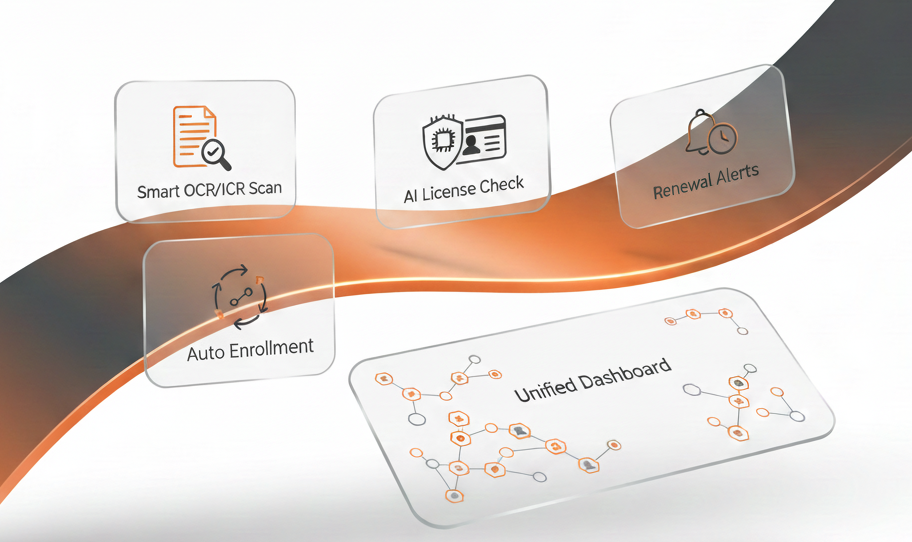
From Application to Approval — Simplified by AI
Faster Enrollment. Higher Accuracy. Better Compliance.
Data Protection That Matches Your Standards
Every credentialing workflow at ValueDX follows HIPAA, SOC 2 and ISO 27001 protocols.
All AI, OCR and ICR processes are encrypted, auditable and traceable — ensuring security, privacy and regulatory compliance
Trusted by 500+ Healthcare Providers
AI That Understands Healthcare Credentialing
Unlike generic automation tools, ValueDX is designed for healthcare credentialing workflows. ValueDX AI understands payer requirements, document formats and revalidation cycles — delivering unmatched accuracy and compliance.
Experience the Power of Healthcare AI Agents Firsthand
Discover how ValueDX AI-powered agents can streamline your credentialing, recredentialing, and provider enrollment processes—reducing administrative burden while improving speed, accuracy, and compliance. Schedule a personalized demo tailored to your platform’s needs:
Fill out the form below and we’ll be in touch to schedule a convenient time.
Let’s explore how intelligent automation can transform your healthcare delivery.
FAQs
Before You Leave…
Discover how our Medical Credentialing & Provider Enrollment services help streamline credentialing, reduce enrollment delays, and ensure compliance.
Request a Free Consultation













