Manual Claims Mean Missed Revenue

Manual Claims Mean Missed Revenue

Discover AI-Powered Healthcare Agents — On Your Terms
Step into the ValueDX AI Experience Center and see how our intelligent automation solutions are transforming healthcare operations. Experience AI agents in action and discover how they simplify workflows, improve patient engagement and optimize revenue cycle management.
From Claim Creation to Payment — Automated by AI
The ValueDX Claims Automation Platform applies AI, machine learning and OCR/ICR document reading to simplify the claims process. AI engine validates data, matches payer rules and auto-corrects errors before submission ensuring clean, compliant claims every time.
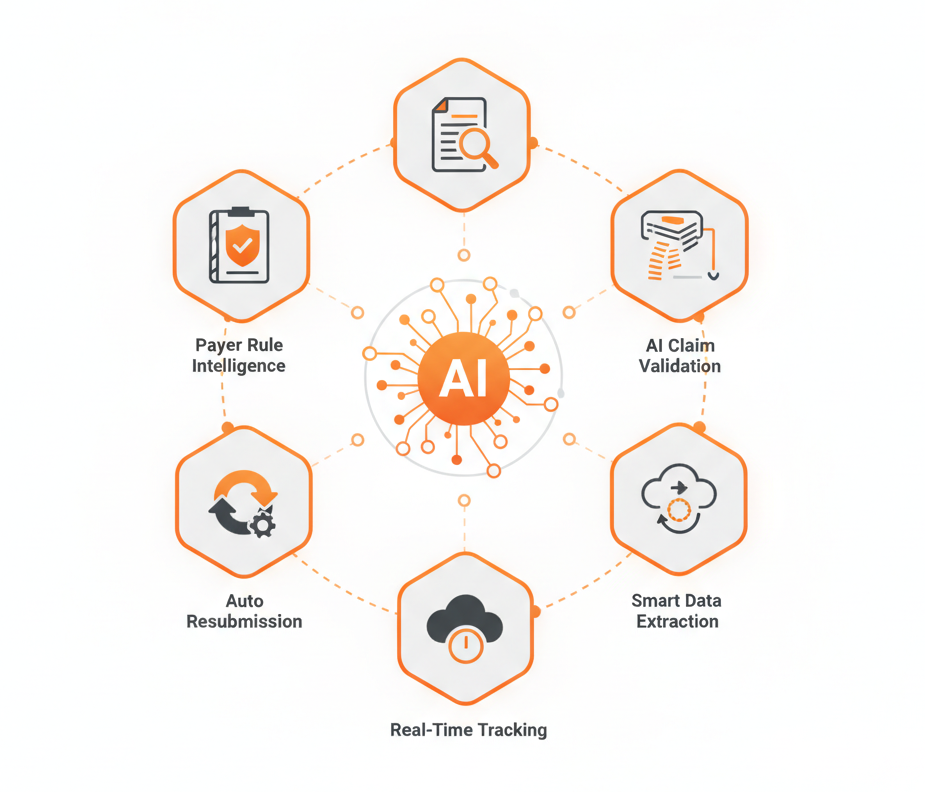
Intelligent Workflow for Claims Perfection
Measure the Impact of Intelligent Claims Automation

Measure the Impact of Intelligent Claims Automation

Purpose-Built AI for Healthcare Revenue Teams
ValueDX isn’t a generic automation tool, it’s a healthcare-expert AI engine that understands payer logic, CPT/ICD codes and claim formats across all major insurers.
Purpose-Built AI for Healthcare Revenue Teams
ValueDX isn’t a generic automation tool, it’s a healthcare-expert AI engine that understands payer logic, CPT/ICD codes and claim formats across all major insurers.
Built for Healthcare Data Integrity
ValueDX ensures every claim workflow is HIPAA, SOC 2 and ISO 27001 compliant. All data processed through AI, OCR or ICR is fully encrypted and auditable — protecting sensitive financial and patient information end to end.
Experience the Power of Healthcare AI Agents Firsthand
Discover how ValueDX AI-powered agents can streamline your healthcare operations, reduce administrative burden and elevate patient experiences. Schedule a personalized demo tailored to your organization’s needs:
Fill out the form below and we’ll be in touch to schedule a convenient time.
Let’s explore how intelligent automation can transform your healthcare delivery.
FAQs
Before You Leave…
Discover how our Claims Processing & Claims Management Submission solutions speed approvals, reduce denials, and improve revenue cycle efficiency.
Request a Free Consultation
