AI Insurance Eligibility Verification Agent — Instant Coverage Checks, Fewer Denials, Cleaner Claims
Every denied claim traces back to a single breakdown — unverified coverage before service delivery. ValueDX’s AI Eligibility Agent closes that gap by connecting directly to payer networks, validating benefits in real time, and writing clean data back to your billing system before a single charge is posted. No manual portal checks. No coverage surprises. No avoidable rejections.
Why Manual Insurance Eligibility Verification Keeps Costing Healthcare Teams
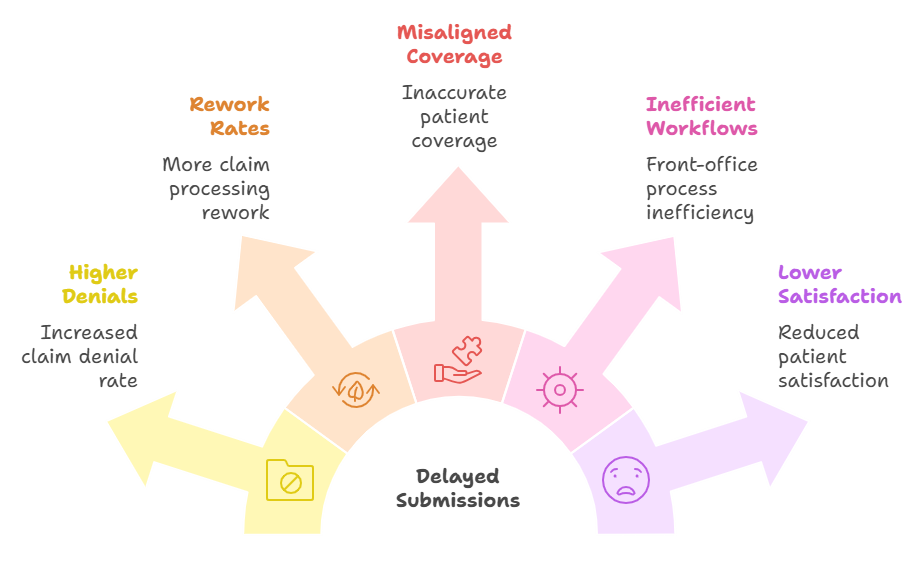
Insurance eligibility verification sounds straightforward — confirm coverage, confirm benefits, move on. But in practice, healthcare billing teams spend an average of 15 to 20 minutes per patient cycling through payer portals, only to discover mid-revenue cycle that coverage lapsed, a plan changed, or a required authorization was missed. Those minutes multiply into hours, those hours into staffing costs, and those staffing costs into denied claims that arrive weeks after the fact — often past the appeal window.
Discover AI-Powered Healthcare Agents — On Your Terms
The ValueDX AI Experience Center gives your team a hands-on look at how eligibility verification actually works inside our platform — not a slide deck, not a scripted walkthrough. Watch the agent pull live patient data, ping payer networks, surface coverage discrepancies, and sync verified results back into a connected EHR — all without a single human keystroke. If you have been evaluating automation vendors, this is where claims get tested against reality.
How AI-Powered Insurance Eligibility Verification Works — Step by Step

Eligibility verification is not just an administrative checkbox — it is the financial control point where revenue cycle performance is either protected or eroded. When coverage is confirmed before a claim is written, everything downstream moves faster and more accurately. When it is guessed at, delayed, or skipped, the result is a cascade of eligibility-related denials, corrective rework, and cash flow disruption.
Meet the ValueDX AI Eligibility Agent — Your Automated Coverage Intelligence Engine
Unlike rules-based eligibility tools that simply ping a payer and return a binary active or inactive status, the ValueDX AI Eligibility Agent performs layered validation. It retrieves current patient demographics from your scheduling system, maps them against active payer contracts, checks plan-specific benefit structures, detects coverage gaps or coordination-of-benefits requirements, and pushes a complete, verified data set back into your billing workflow — typically within seconds of an appointment being booked or modified.
End-to-End AI Eligibility Verification — What Happens at Every Step
Here is exactly what the ValueDX AI Eligibility Agent does from the moment a patient appointment is created to the moment a verified, clean record lands in your billing queue:
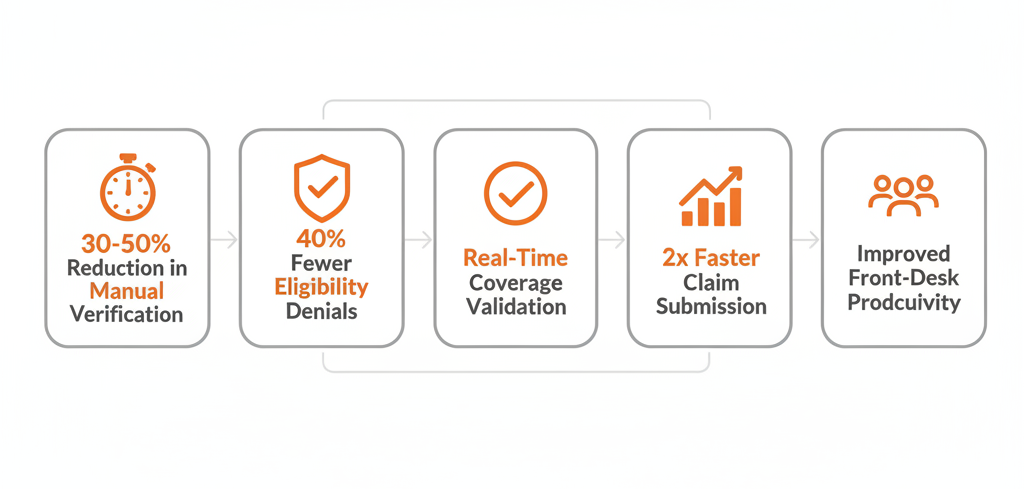
Measurable Results from Automated Insurance Eligibility Verification
HIPAA-Compliant Insurance Eligibility Verification — SOC 2 Type II & ISO 27001 Certified
Security in healthcare data workflows is a baseline requirement. ValueDX’s AI Eligibility Agent is built to meet that standard, with all data encrypted in transit using TLS 1.2+ and at rest using AES-256. Access is controlled through role-based permissions, with audit logs tracking every action, including timestamps and user details. ValueDX is compliant with HIPAA, SOC 2 Type II, and ISO 27001, and provides audit documentation on request. State-specific compliance configurations are also available if needed.
Built Specifically for Healthcare Eligibility Verification — Not Adapted from Generic Automation
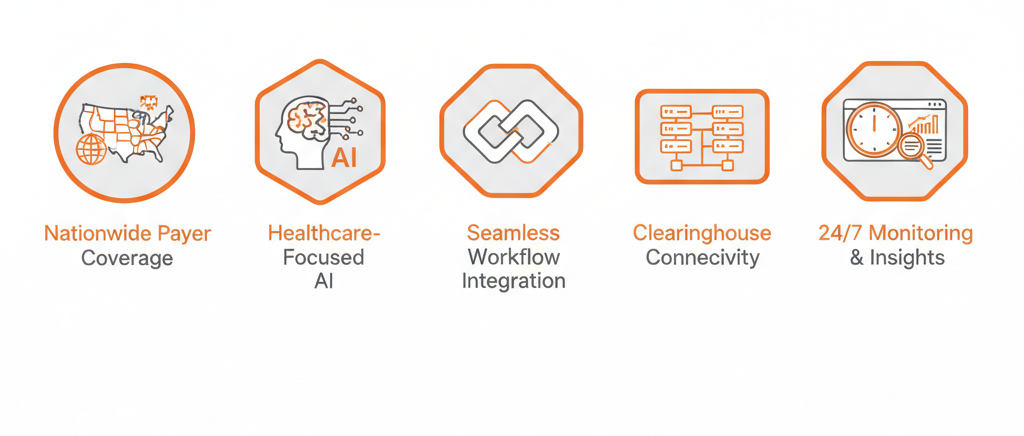
EHR, PMS, and Clearinghouse Integration for AI Insurance Eligibility Verification
Most eligibility failures are not technology failures — they are integration failures. Data sits in the EHR, verification happens in a separate portal, and the result gets manually re-entered into the billing system. Three systems, two manual handoffs, and multiple opportunities for data loss. ValueDX eliminates all three transfer points. The AI Eligibility Agent integrates natively with Epic, Cerner, Athenahealth, eClinicalWorks, Allscripts, and most major PMS platforms using standard HL7 FHIR and X12 270/271 EDI protocols. Verification results flow back into your system of record automatically — no copy-paste, no upload, no reconciliation step.
Experience the Power of Healthcare AI Agents Firsthand
See how ValueDX AI-powered agents can transform your healthcare platform—reducing administrative burdens, elevating patient experience, and accelerating cash flow.
With deep integrations across EHRs, payers, and clearinghouses, our AI agents empower data-driven decisions and proactive revenue intelligence for sustainable growth.
Fill out the form below and we’ll be in touch to schedule a convenient time.
Let’s explore how intelligent automation can transform your healthcare delivery.
Frequently Asked Questions — AI Insurance Eligibility Verification
Start Verifying Patient Insurance in Real Time — Schedule Your Personalized Demo
The ValueDX AI Eligibility Agent changes that calculation. We will walk you through a live demonstration using real payer connections, show you exactly where your current verification workflow breaks down, and map out what a deployment would look like inside your specific EHR and payer mix. No obligation. No generic slide deck. Just a clear picture of what automated eligibility verification looks like for your facility.

